Welcome to the 94th Emerge Australia Research Digest, where you will find summaries of some of the latest research and information about ME/CFS, with links to the complete articles.
You can also join our community and choose to have the Digest delivered straight to your inbox at the end of every month, by signing up to our mailing list here.
We appreciate the support of everyone who reads the Digest – we encourage regular subscribers to support us with a monthly suggested donation of $2. You can sign up for monthly giving here.
Recovery from Exercise in Persons with Myalgic Encephalomyelitis/Chronic Fatigue Syndrome (ME/CFS)
Authors: Moore GE, Keller BA, Stevens J, Mao X, Stevens SR, Chia JK, … Hanson MR (Cornell University, USA)
Publication: Medicina
Link: https://pubmed.ncbi.nlm.nih.gov/36984572/
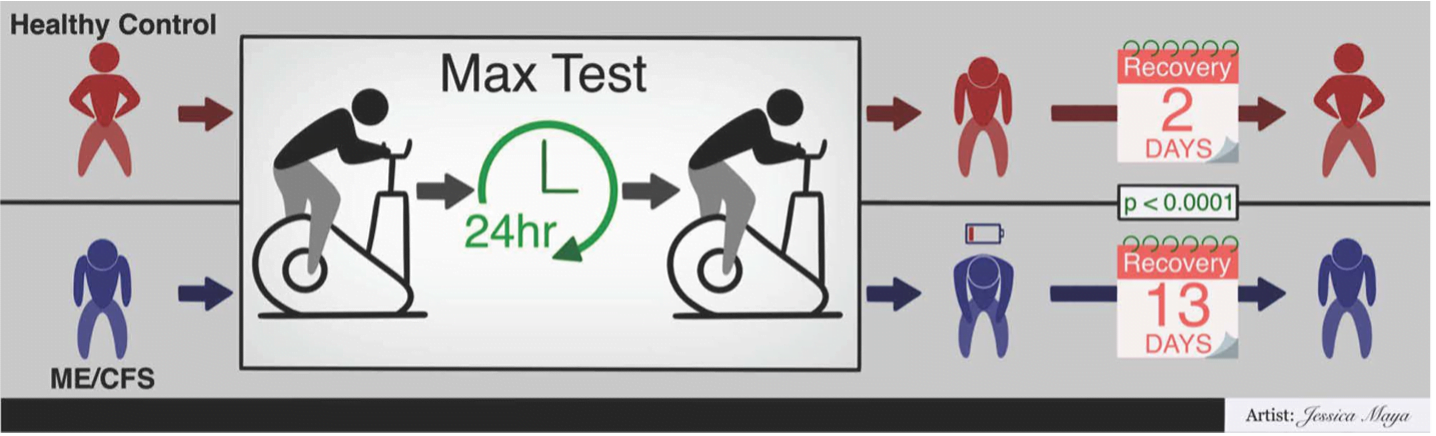
Two-day cardiopulmonary exercise tests (2-day CPET) are commonly used to elicit and measure physiological responses to exercise in ME/CFS. These authors tracked post-exercise symptom severity following 2-day CPET in ME/CFS to examine the exercise dose-recovery response relationship.
Eighty people with ME/CFS (Canadian Consensus Criteria) and 64 healthy, sedentary controls, underwent a 2-day CPET. Participants’ performance met maximal effort criteria. Post-exertional symptoms were monitored using the Specific Symptom Severity (SSS) questionnaire, which has nine domains: fatigue, brain fog, sore throat, tender lymph nodes, myalgia, arthralgia, headache, disturbed sleep and post-exertional malaise (PEM). SSS scores were obtained immediately prior to the first CPET, 24 hours after the second CPET, and then every two days for ten days after the first CPET, or until symptoms returned to baseline.
The difference in judged recovery time between the ME/CFS and control groups was highly significant. Recovery time ranged from 1-64 days in the ME/CFS group, and from 1-10 days in the control group, with an average of 12 days for ME/CFS and two days for controls. Illness duration and severity of baseline symptoms did not affect recovery time.
The authors adapted pharmacokinetic modelling to examine the dose-response relationship to exercise in ME/CFS, utilising time to peak effect, the magnitude of peak effect and time to decay. The modelling showed that the decay rate of post-exertional symptoms in ME/CFS is extremely prolonged.
The authors conclude that their data suggest that “graded exercise therapy almost certainly would cause harm. Small wonder, therefore, that graded exercise therapy has fallen into disfavour in the ME/CFS community”. They suggest that their pharmacokinetic modelling could be very useful for clinicians
managing ME/CFS and PEM.
Two symptoms can accurately identify post-exertional malaise in myalgic encephalomyelitis/chronic fatigue syndrome
Authors: Davenport TE, Chu L, Stevens SR, Stevens J, Snell CR, Van Ness JM (Workwell Foundation, USA)
Publication: Work
Link: https://content.iospress.com/articles/work/wor220554
While post-exertional malaise (PEM) is the core feature of ME/CFS, its diversity of presentation, clinicians’ lack of familiarity with the symptom and the lack of clinically useful tools to assess PEM, hamper the ability of clinicians to diagnose ME/CFS. These researchers set out to identify a clinical prediction rule that would allow clinicians to quickly and easily identify if their patients experience PEM.
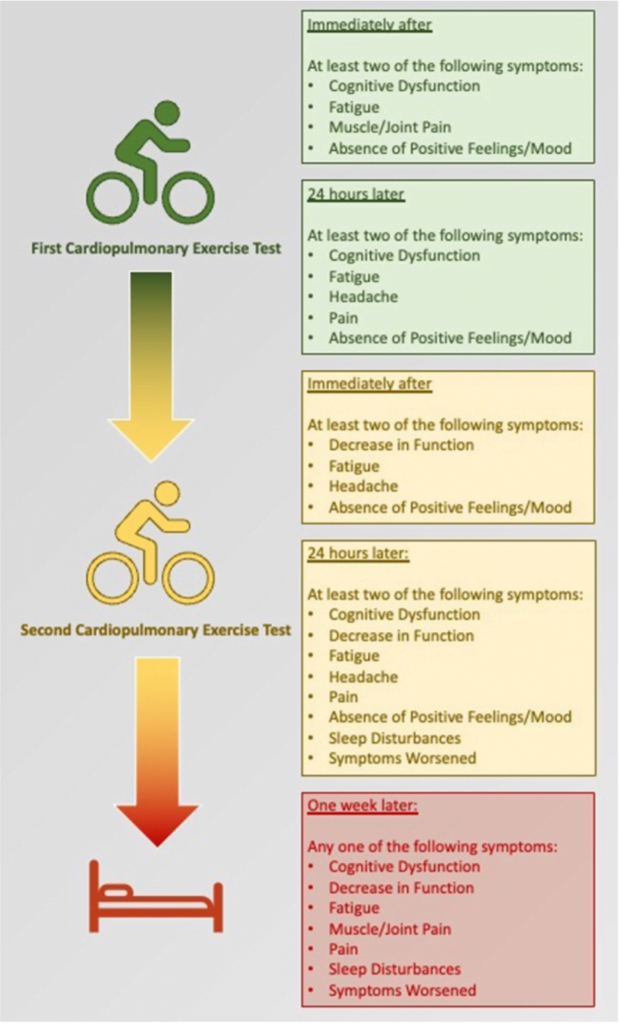
The study included 49 participants with ME/CFS (Fukuda criteria) and 10 healthy, sedentary controls (HC). All participants underwent two maximal cardiopulmonary exercise tests (CPET) conducted 24 hours apart. Participants completed an open-ended questionnaire about how they felt, and symptoms experienced at five time points: immediately after CPET 1, 24 hours after CPET 1, immediately after CPET 2, 24 hours after CPET 2, and 7 days after CPET 2. Responses were coded and analysed to identify which symptom reports were sufficient to differentiate the two groups.
ME/CFS participants reported significantly more symptoms (19.2) than HC (7.1) and took significantly longer to recover from the exercise tests (49% reported an average of 4.5 days to recovery, while the remaining 51% had not recovered after seven days. HC all recovered within one day or less). At all time periods, a maximum of two symptoms were optimal to differentiate between ME/CFS and HC, with only one symptom necessary to differentiate the two groups at 7 days. Fatigue, cognitive function, loss of positive mood and decrease in function were consistent predictors of ME/CFS at all time points.
The authors note that, while post-exertional loss of function is repeatedly reported by patients and is also included in the National Academy of Medicine diagnostic criteria, there is not a widespread emphasis on this impact of PEM. They note that a combination of patients not always having the language to describe their experience and clinicians not asking directly about function has resulted in this key impact being largely absent from clinical practice and research. They suggest that, in addition to patient reporting, portable monitoring devices (such as actimeters) can be used to measure post-exertional changes in function in clinical settings, especially to monitor the delayed and prolonged nature of PEM.
Exercise Pathophysiology in Myalgic Encephalomyelitis/Chronic Fatigue Syndrome and Post-Acute Sequelae of SARS-CoV-2: More in Common Than Not?
Authors: Joseph P, Singh I, Oliveira R, Capone CA, Mullen MP, Cook DB, … Systrom DM (Harvard University, USA)
Publication: Chest
Link: https://pubmed.ncbi.nlm.nih.gov/37054777/
There are considerable overlaps between post-acute sequelae of SARS-CoV-2 (PASC) and ME/CFS. This review outlines the similarities in underlying exercise pathophysiology in response to both invasive and non-invasive cardiopulmonary exercise testing (iCPET and niCPET respectively). The review focuses on people with PASC and ME/CFS who do not have underlying cardiopulmonary abnormalities and who present with post-exertional malaise (PEM).
Preload failure (low ventricular filling pressure), small fibre neuropathy, impaired systemic oxygen extraction, ventilators inefficiency associated with dyspnoea are commonly seen in iCPET in both PASC and ME/CFS.
While deconditioning has been offered as an explanation for exertional intolerance in both PASC and ME/CFS, the authors argue that results from iCPET studies suggest deconditioning is not the primary cause. Findings of preload failure are opposite to the high ventricular filling pressure found in deconditioning. Peripheral oxygen extraction, while impaired in PASC and ME/CFS, is not significantly affected by deconditioning.
The authors conclude that iCPET offers invaluable insights into exercise pathophysiology in both PASC and ME/CFS, and that further study is needed to both better understand the underlying mechanism of exertional intolerance and to develop potential treatments to reduce PEM and increase exercise tolerance.
Adelaide woman's 'debilitating' long COVID experience published in British Medical Journal
Authors: Hams S
Publication: ABC News
Link: https://www.abc.net.au/news/2023-04-14/long-covid-experience-shared-in-british-medical-journal-research/102217016
Adelaide registered nurse Kim Gibson tested positive for COVID-19 in April last year. Despite only having mild COVID-19, she continues to have debilitating symptoms. She developed hearing loss, tinnitus and vertigo, and it took months for doctors to identify these as rare symptoms of long COVID.
To help inform doctors of these symptoms, Kim worked with University of South Australia researcher, Dr Micah Peters to have her experience documented in BMJ Case Reports.
“We need a better and more comprehensive picture of the long-term effects that can impact on people, in weeks or months or even years later on,” Dr Peters said.
Albanese government pledges $50m for long COVID research as inquiry calls for action
Authors: Lu D
Publication: Guardian Australia
Link: https://www.theguardian.com/world/2023/apr/24/albanese-government-pledges-50m-for-long-covid-research-as-inquiry-calls-for-action
The parliamentary inquiry into long COVID has released its long-awaited report. Recommendations include an injection of $50m into long COVID research, the establishment of an Australian Centre for Disease Control, as well as a coordinated national research program into COVID-19 and long COVID, and support and education for GPs to diagnose and manage long COVID.
The report also includes a recommendation for more research and patient support for those living with ME/CFS.
“It is clear that long Covid is a significant problem and estimates vary, indicating that between 2% to 20% of those infected with Covid-19 may develop long Covid. Even if it is the lower figure of 2%, this is still many people requiring help and support”, the committee Chair, Dr Mike Freelander, said.







