Symptom management cannot treat the underlying cause of ME/CFS or long COVID, but it can help improve quality of life by reducing the severity of symptoms.
Many people with ME/CFS are sensitive to medications. You may wish to talk with your doctor about starting at a very low dose and increasing slowly over time. This is often called a “start low, go slow” approach.
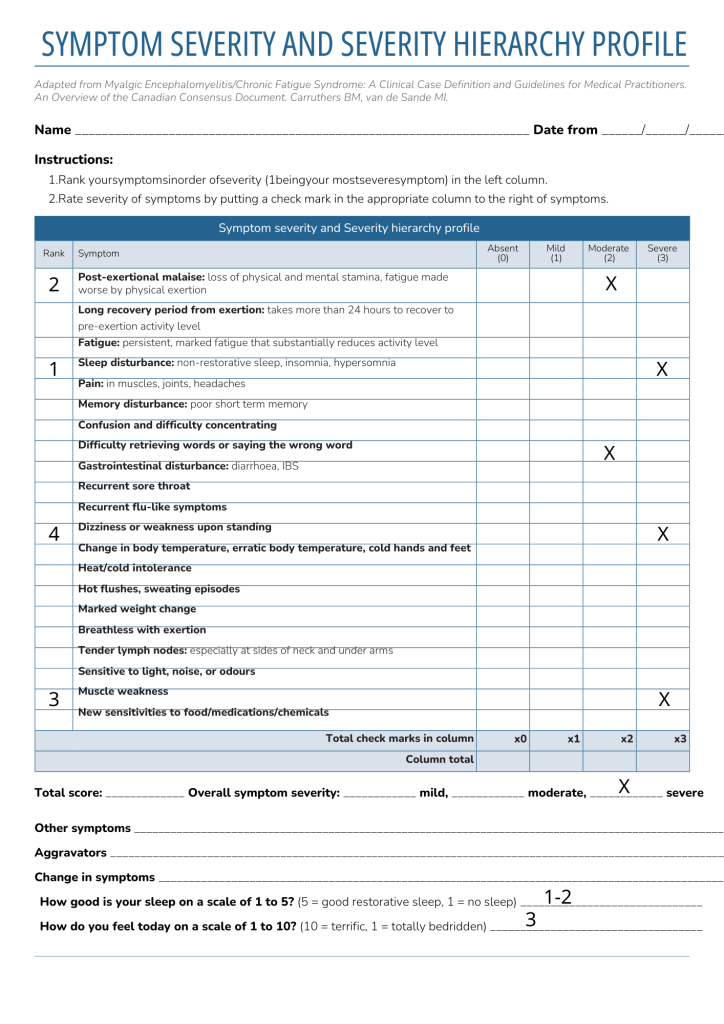
Tracking symptoms can feel overwhelming for people living with ME/CFS or long COVID. To make this easier, we recommend using the Symptom Severity and Severity Hierarchy Profile. This tool helps give your doctor a clear and simple overview of your symptoms.
Using the profile involves:
- Ranking your symptoms from most to least problematic
- Looking at ways to reduce symptoms, starting with the most difficult ones
You can download a copy of the chart by clicking here.
When completing the Symptom Severity and Severity Hierarchy Profile:
- Think about how severe your symptoms have been over the past two to four weeks.
- You may choose to fill in one profile for an average day and one for a worst day.
- Note how many average days and how many worst days you have had in the past two weeks.
- This is your personal profile. It should reflect how you experience your symptoms. It is not about comparing yourself to others or predicting future changes.
- If your doctor is willing, ask them to sign the document and add it to your medical record. This may be helpful in the future if you need evidence of long-term symptom management.
- You may also choose to complete a new profile in six to twelve months to compare changes in your health or treatment outcomes.
Over time, this can help you understand your functional baseline. Your functional baseline is the amount of physical, mental, and emotional energy you can use without triggering PEM or worsening your health. Finding your baseline can take time, but once known, it can guide how you manage your condition.